Samuel Borges Photography/ Shutterstock
Susan Walker, Anglia Ruskin University
Breast cancer is one of the most common types of cancer worldwide, with around 2.3 million women diagnosed with the disease every year. In the UK alone, it is estimated that one in seven women will develop breast cancer at some point in their lifetime.
The biggest determinants for developing breast cancer are age and being female. But other lifestyle factors, such as weight, how much you drink, whether or not you exercise, and hormone levels, can also play a smaller part in elevating your risk.
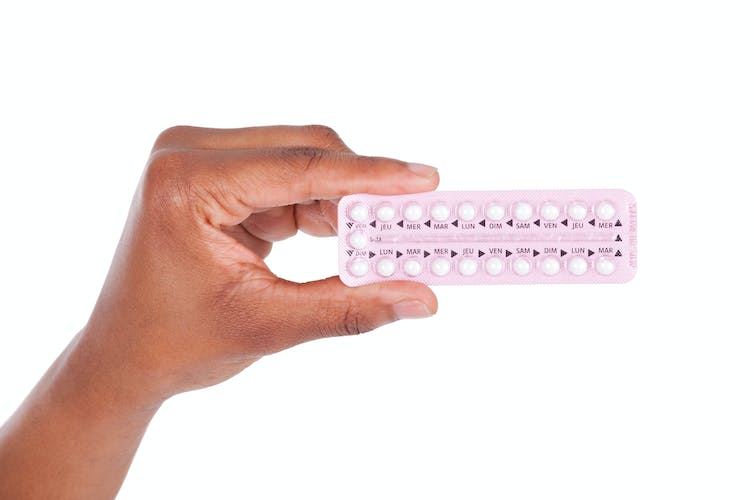
It has also been known for many years now that women who are using or have recently used the combined oral contraceptive pill for more than five years have a 25% greater risk of developing breast cancer compared to their risk if they hadn’t taken the pill. But despite this small increase in risk, only about 1% of all breast cancers in the UK are linked to the use of oral contraception.
Until now, it was thought that only the combined hormonal pill carried a greater risk of breast cancer. But a recent study suggests that the progestogen-only pill (also known as the mini pill) and other forms of hormonal contraception also carry the same increase in breast cancer risk as the combined pill.
The authors of the study looked at data from the GP records of more than 27,000 women in the UK, and combined this with data from 12 other published studies that had looked at the effect of different types of hormonal contraceptives (including the progesterone-only pill, hormonal IUDs, the implant and the injection) on breast cancer risk.
With this data, they were able to estimate whether women who had been diagnosed with breast cancer under the age of 50 were more likely to have used various forms of hormonal contraceptives, compared to women of the same age who had not been diagnosed with breast cancer. The study took into account other factors that may affect risk of breast cancer, such as body weight, alcohol intake and whether they had children.
The study found women who used progestogen-only hormonal contraceptives had between a 20-30% greater risk of developing breast cancer compared to women not using these methods. This increased risk disappeared ten years after stopping the method.
Making individual choices
To better put the study’s findings into perspective, it might help to look at the extra number of people who may develop breast cancer due to having used hormonal contraceptives, compared to the number of women who will develop breast cancer without having used birth control.
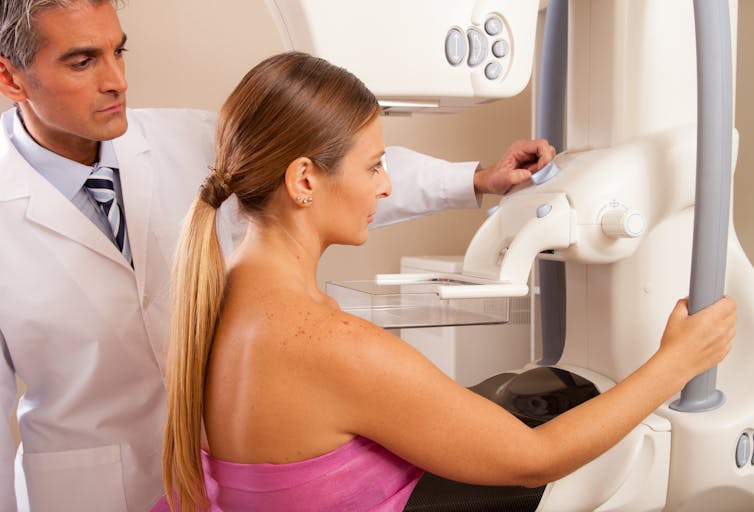
GagliardiPhotography/ Shutterstock
So for example, the researchers in this study estimate that in a group of 100,000 women aged 35-39, about 2,000 women will develop breast cancer over a 15-year period due to a range of factors unrelated to the use of hormonal contraception. But given that the study found birth control carries between a 20-30% greater risk of developing breast cancer, they estimate that an additional 265 women will therefore develop breast cancer over a 15-year period as a direct results of taking oral birth control.
If we were to look at women aged 50-54, we know from other research that about 280 women per 100,000 are diagnosed with breast cancer each year. If birth control increases breast cancer risk by 20-30%, it would mean an additional 70 women per 100,000 would develop breast cancer each year.
This is one of the reasons women are not advised to take the combined pill over the age of 50. The results of this latest study mean women may also want to consider the slightly increased risks of breast cancer with progestogen-only contraceptives over the age of 50. However, progestogen-only methods remain safer in terms of cardiovascular risks – such as stroke and heart attacks – in this age group.
Obviously, breast cancer is a serious disease and a leading cause of death in younger women, so anything which increases a person’s risk of breast cancer has to be considered carefully.
But one of the difficulties of deciding on whether a contraceptive method presents an acceptable risk is that many other common lifestyle behaviours also increase cancer risk. For example, it’s estimated that while 1% of breast cancers in the UK are caused by hormonal contraceptives, 5% are caused by not breastfeeding, 8% by being overweight and 8% by drinking alcohol.
This is further complicated by the fact that hormonal contraceptives can have some benefits. For example, the contraceptive injection can help ease symptoms in women who have endometriosis, while the intrauterine device is very effective in treating very heavy periods.
The combined oral pill reduces the risk of endometrial cancer by about 50% and ovarian cancer by about 40%. It’s also beneficial in helping with hot flushes and other pre-menopausal symptoms. Not to mention that contraception allows a woman to control her reproductive cycle and avoid unwanted pregnancy.
The decision about which contraceptive method to use is an extremely personal choice. The findings of this study provide important clarity on breast cancer risk, allowing women to make a more informed decision when it comes to using contraception.![]()
Susan Walker, Reader in Contraception, Reproductive and Sexual Health, Anglia Ruskin University
This article is republished from The Conversation under a Creative Commons license. Read the original article.